Baltimore, MD—The buildup of scar tissue makes recovery from torn rotator cuffs, jumper’s knee, and other tendon injuries a painful, challenging process, often leading to secondary tendon ruptures. New research led by Carnegie’s Chen-Ming Fan and published in Nature Cell Biology reveals the existence of tendon stem cells that could potentially be harnessed to improve tendon healing and even to avoid surgery.
“Tendons are connective tissue that tether our muscles to our bones,” Fan explained. “They improve our stability and facilitate the transfer of force that allows us to move. But they are also particularly susceptible to injury and damage.”
Unfortunately, once tendons are injured, they rarely fully recover, which can result in limited mobility and require long-term pain management or even surgery. The culprit is fibrous scars, which disrupt the tissue structure of the tendon.
Working with Carnegie’s Tyler Harvey and Sara Flamenco, Fan revealed all of the cell types present in the Patellar tendon, found below the kneecap, including previously undefined tendon stem cells.
“Because tendon injuries rarely heal completely, it was thought that tendon stem cells might not exist,” said lead author Harvey. “Many searched for them to no avail, but our work defined them for the first time.”
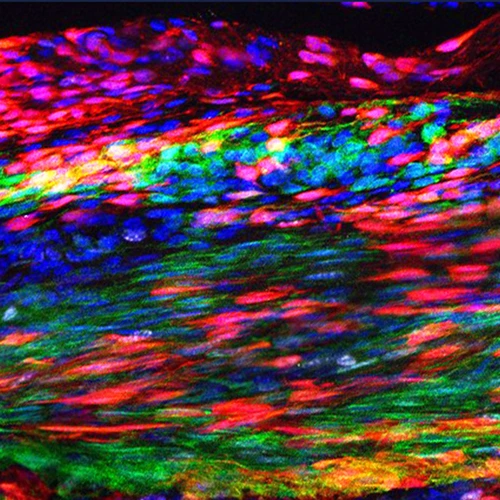
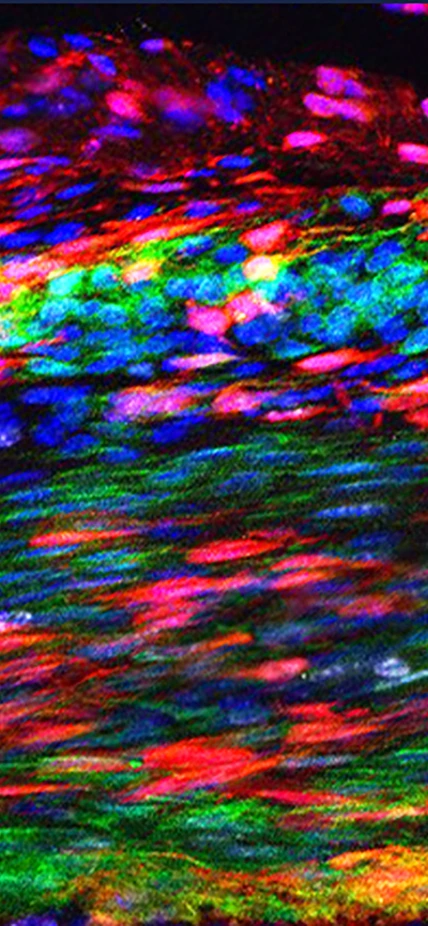
Image: The Patellar tendon 30 days after injury. The red marks newly discovered tendon stem cells that have self-renewed and are layered over green marked original tendon cells. During regeneration, some tendon stem cells differentiate to make newly regenerated tendon cells — a process during which they transition into a yellow-orange color. The blue indicates cellular nuclei. Courtesy of Tyler Harvey.
Stem cells are “blank” cells associated with nearly every type of tissue, which have not fully differentiated into a specific functionality. They can also self-renew, creating a pool from which newly differentiated cell types can form to support a specific tissue’s function. For example, muscle stem cells can differentiate into muscle cells. But until now, stem cells for the tendon were unknown.
Surprisingly, the team’s research showed that both fibrous scar tissue cells and tendon stem cells originate in the same space—the protective cells that surround a tendon. What’s more, these tendon stem cells are part of a competitive system with precursors of fibrous scars, which explains why tendon healing is such a challenge.
The team demonstrated that both tendon stem cells and scar tissue precursor cells are stimulated into action by a protein called platelet-derived growth factor-A. When tendon stem cells are altered so that they don’t respond to this growth factor, then only scar tissue and no new tendon cells form after an injury.
“Tendon stem cells exist, but they must outcompete the scar tissue precursors in order to prevent the formation of difficult, fibrous scars,” Fan explained. “Finding a therapeutic way to block the scar-forming cells and enhance the tendon stem cells could be a game-changer when it comes to treating tendon injuries.
This work was supported by the U.S. National Institutes of Health.